
Sometimes the unexpected is inconvenient. That’s why we have services available after hours at convenient locations. Unlike many other urgent care centers, we’re here for you past the usual nine-to-five, including specific pediatric services at some of our locations for a road to quick recovery. An urgent care location isn’t an emergency room, but we’re well-prepared to help you with minor accidents, sudden illnesses, and unexpected events that throw life off track.
Many of our providers offer telehealth appointments as an opportunity for patients who aren’t able to visit the clinic themselves or where it otherwise makes more sense. From sinus infections to a follow-up appointment, telehealth is a convenient tool to make your health easy for you to prioritize. After an initial visit with one of our specialists, we often like to offer additional appointments to make sure things are running smoothly. Ask your doctor about how telehealth could be an option for you.


A physician-owned healthcare company in Davis County dedicated to patient-focused services, Tanner Clinic’s mission is your wellbeing. Our providers bring innovative and comprehensive care to our multiple locations. As a leading healthcare provider in northern Utah, we exceed patient expectations with accessible, compassionate, helpful care. Alongside our thriving Family, Internal Medicine and Pediatric practices, we also provide specialized care in nearly any field, many not always found in other area clinics. With exemplary physicians and staff who dedicate themselves to an environment of honesty and respect, Tanner Clinic is a community-driven collection of people who really care about you and your health. Book an appointment with one of our many specialty or primary care providers today!
Many of our providers are available via our patient portal to refill medical prescriptions or ask a quick question. Through the patient portal, you can also save yourself a trip up to the clinic or a battle with paperwork to obtain medical records for insurance or personal use. The portal is an incredibly convenient tool for many of our patients, so be sure to ask your provider after booking your appointment whether or not it’s available for you to use.
Easily pay your medical bills online with our online bill service! Besides making the process of paying your bills that much easier, this service also allows you to see your Tanner Clinic e-statements and billing history. With all the information you would need to know about your visits to our clinic just a click away, your medical care will be a simplified and worry-free experience.
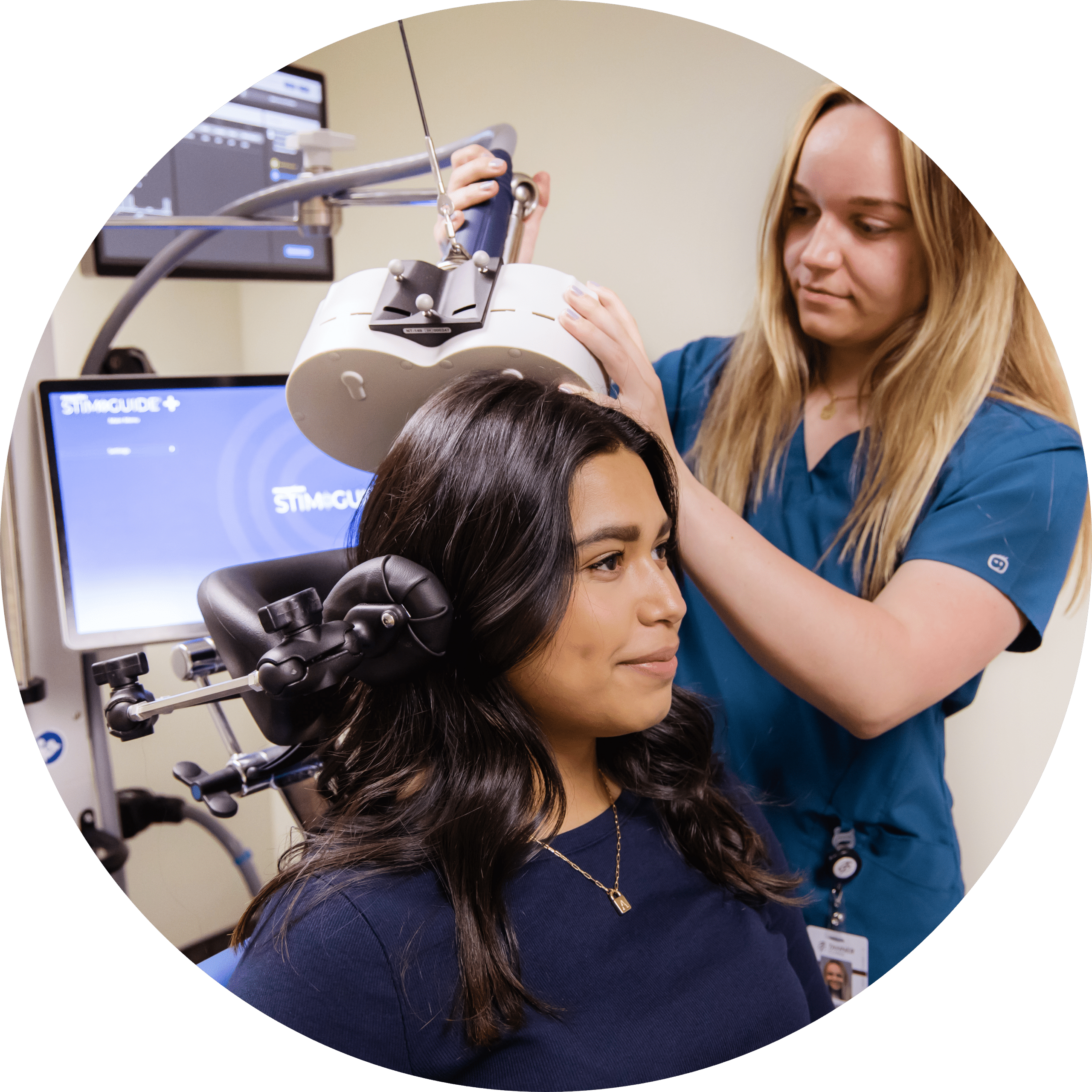
The relationship between emotions, thoughts, and mental well-being is what behavioral health addresses. With our highly-trained team of psychiatrists, health psychologists, neuropsychologists, therapists and eating disorder specialists, we are making innovative strides forward into behavioral health fields. When we take into account life factors like mental health concerns, relationships, and physical health factors, we get a greater understanding of what might be causing tension or unrest in your life. Through diagnosis and treatment, we’re able to bring you forward into a healthy and happy future.
A few of the most prevalent of the conditions in which our providers specialize include:
We’re constantly looking for the best way to serve in the evolving world of behavioral health. From our East Layton eating disorder clinic to our revolutionary transcranial magnetic therapy, we are treating behavioral health needs in Davis County one step at a time. Reach out to us to schedule an appointment today to find your way to a better mental health. Find a neurologist for nerve pain at Tanner Clinic.

With providers located in Layton, Syracuse, Kaysville, our dermatology care is focused on what you as the patient needs most. Whether rosacea, chronic acne, or something more serious like skin cancer or eczema, we have a specialist prepared to treat you and help your skin back to a healthy state. Our specialists address medical and surgical solutions for skin, hair, and nail problems, both diseases and cosmetic. From pediatric dermatology to skin issues that affect young adults and all the way to advanced dermatology, you’ll find the answers your skin needs here at Tanner Clinic.
Acne treatment is by far the most common dermatological condition we treat, and we’ve seen significant improvements for our patients’ skin appearance and overall health. Since acne treatment finds the underlying cause of the blemishes, we’re able to attack the issue at its source and build a healthy foundation for your skin moving forward.
Along with acne treatment, we also serve patients who have skin cancer, psoriasis, and mole removal.
Even beyond these common diseases, a dermatologist can help you improve the appearance of your skin in several ways:
If any of these specialties sound like an answer to your skin’s needs, be sure to reach out to Tanner Clinic today and schedule an appointment for individualized care and long-lasting results.
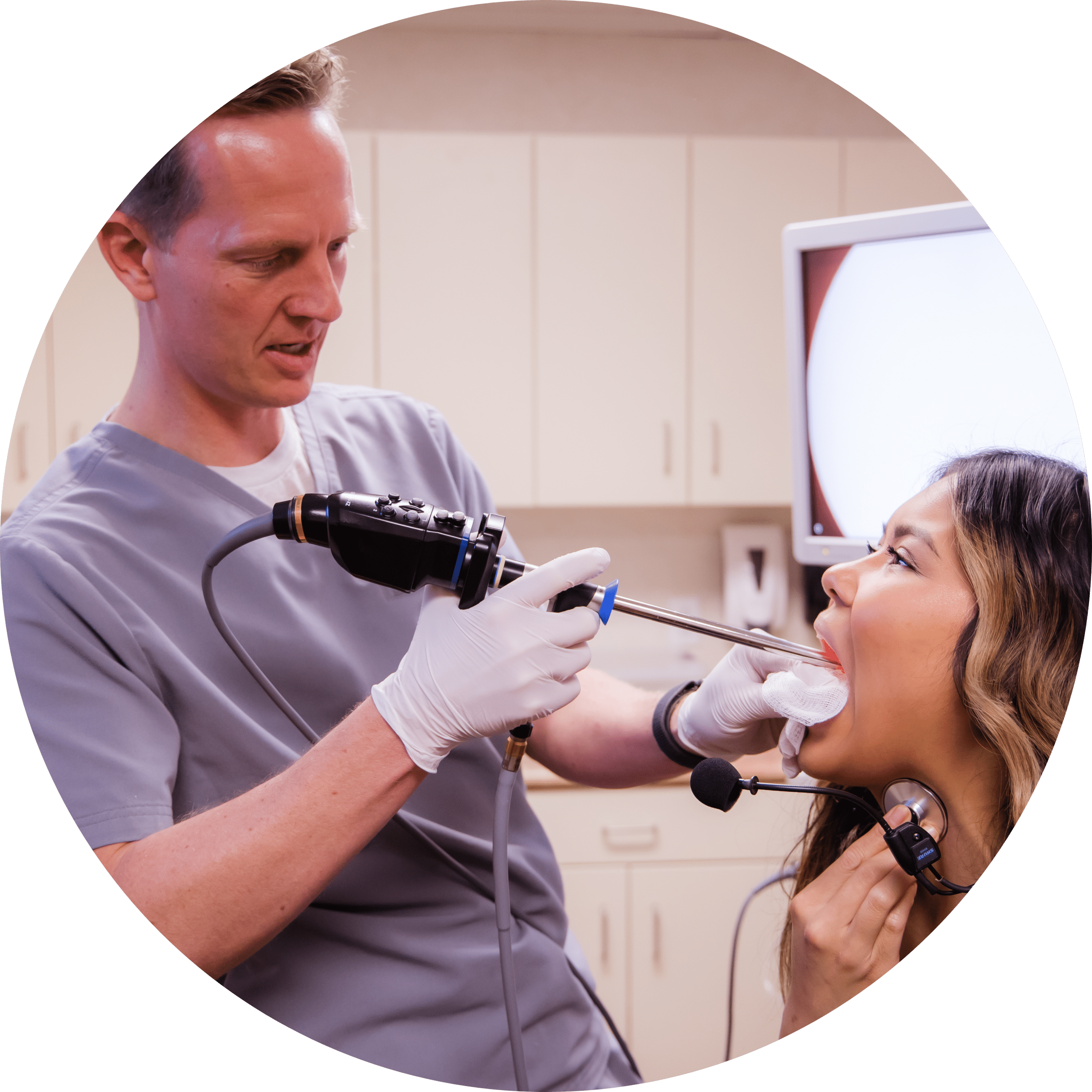
Our otolaryngologists (ear, nose, and throat doctors) prioritize evaluation and quality treatment when it comes to disorders of the ears, nose, and throat. From simple, common issues to more complex disorders, we have specialists who are able to meet every otolaryngological need. At Tanner Clinic, we have state-of-the-art medical and surgical services not only for basic illnesses of the ear, nose, and throat, but also for more complicated issues. Some of the areas that ENT disorders can affect include:
Contact our main Layton location today to schedule an otolaryngological appointment.
With constant training and certifications keeping them at the forefront of their field, our ENT providers are well-equipped with recent innovations and medical research for ENT conditions. Providers at our clinic will often work with audiologists and voice therapists for hard of hearing patients, those experiencing hearing loss, and patients receiving hearing tests for hearing aids. Many of our otolaryngologists also specialize in the diagnosis and treatment of allergies, so if your ENT condition is connected to an underlying allergy, they’ll be able to address that with relevant expertise.
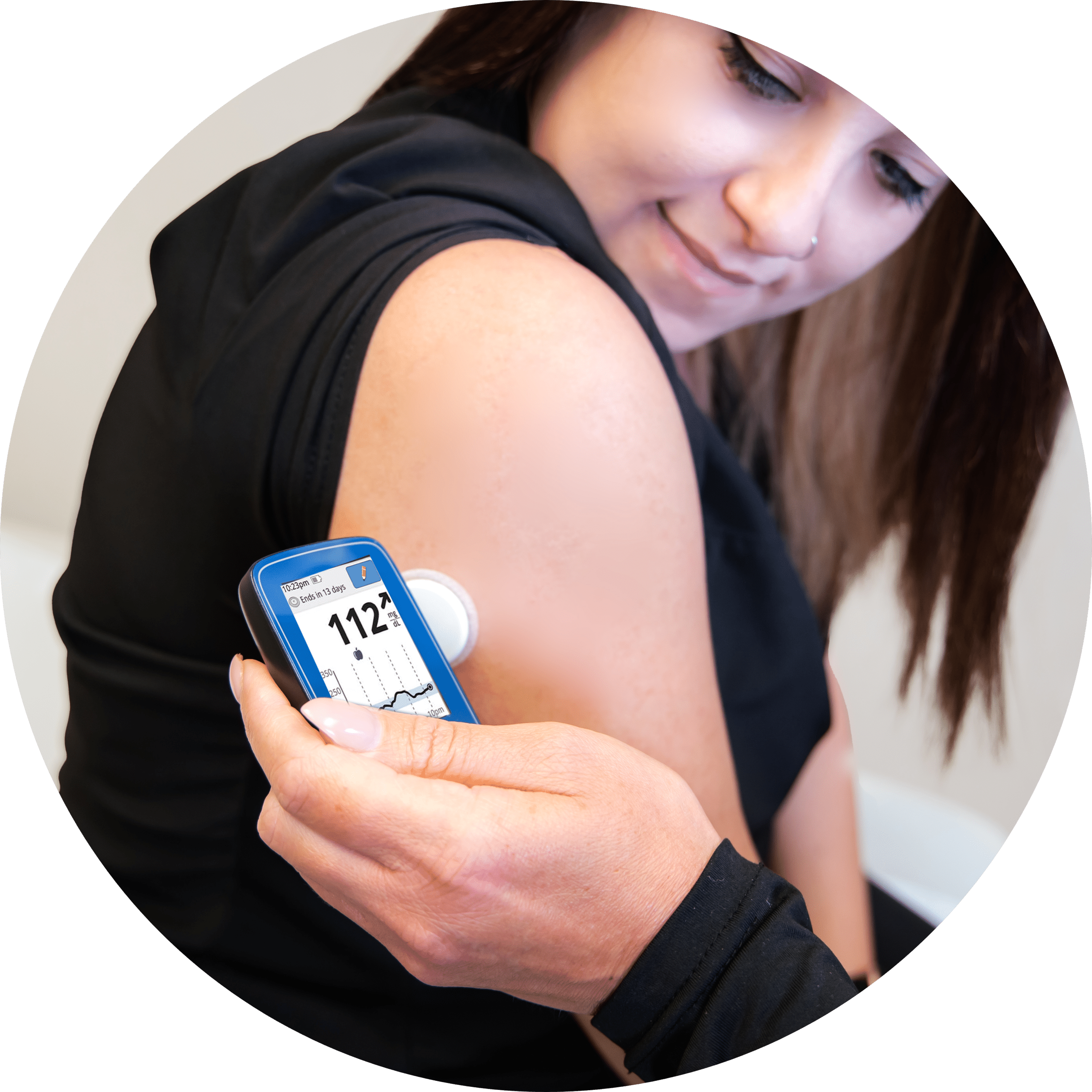
Tanner Clinic offers endocrinology treatment for hormone-related diseases. Our endocrinologists work with the latest technology to diagnose and treat hormone problems and the complications that arise from them. Working with our team of medical specialists and doctors, you can find ways to help manage your illness. Feel healthier and happier with Tanner Clinic. Book an appointment with one of our endocrinology specialists today.
You might want to see an endocrinologist if you experienced any of the following conditions: menopause, diabetes, metabolic disorders, lack of growth, osteoporosis, thyroid diseases, reproductive diseases, hypertension, and infertility. Any of these conditions, along with other symptoms, are an indicator to have your endocrine system checked. Upon the first visit with our endocrinologists, you will get a thorough checkup of your entire body, including your hormone levels. Following diagnosis, our endocrinologists will suggest a treatment plan depending on which underlying condition is causing your symptoms.

Family medicine is a broad term that covers the comprehensive care of both adults and children. This general practice provides a foundation for Tanner Clinic’s care, and our families are among our most prevalent and diverse patient groups. Within our team, family medicine physicians provide care for conditions like:
Family practitioners coordinate care with other medical professionals so that your children and you yourself are always being cared for by informed and prepared providers. When you visit a family medicine doctor for non-emergency health concerns, routine screenings, and yearly physicals, you’re setting the foundation of information in the event that more serious issues arise. And, with immunizations, labs, cholesterol and blood sugar testing through your family medicine doctor, you’re decreasing the likelihood of a serious medical condition arising unnoticed.
One of the main elements of family medicine is the role of your doctor as a primary care physician (PCP). Our family doctors and internal medicine doctors at our family medicine clinic in Layton, Utah become PCP for patients. Finding a PCP is crucial to your preparedness for any emergencies and a cohesive follow up with your health concerns. Bouncing from one provider to another doesn’t provide the best care for you as a patient; that’s why establishing a PCP you can trust is advised and necessary in order to have all of your medical needs met. Many insurance plans require referrals from your established PCP before they will cover visits from a specialist. As this practice increases, it’s wisest for all families in Layton to find a family medical provider they can depend on to label as their PCP to avoid any hassle when a specialist might be a necessary next step.
Tanner Clinic offers gastroenterology care through our providers at Utah Digestive Health. With offices in Layton and South Ogden, these physicians and staff have a 20+ year reputation of premiere digestive care in Utah.
Our gastroenterologists provide patients with quality care and solutions for several digestive disorders. GI patients with our providers have access to specific testing and customized treatment plans to care for digestive disorders such as:
Irritable Bowel Syndrome
With personalized care and valuable specialists who know their fields well, your gut health will be the priority when you book an appointment with Tanner Clinic.
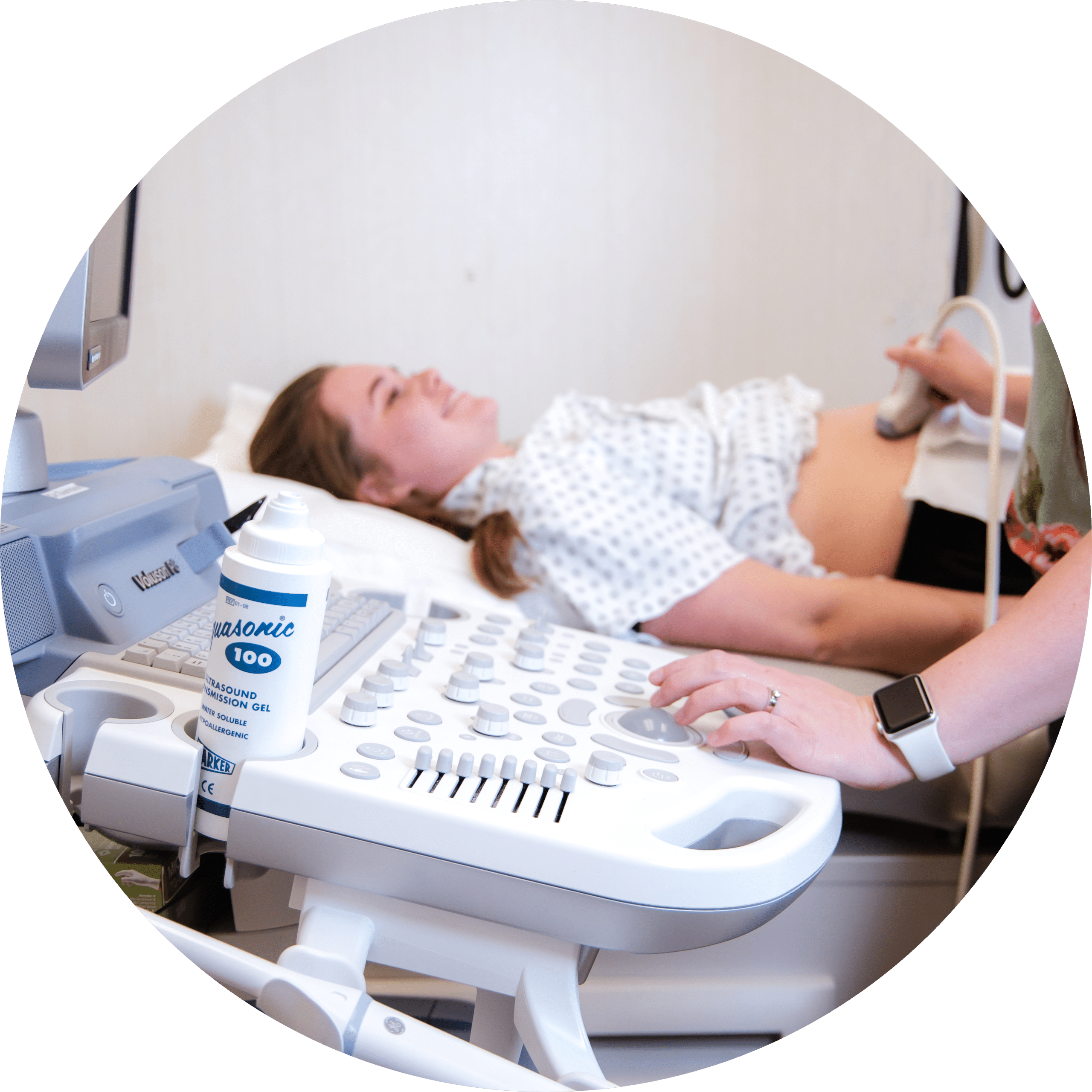
If you need an annual exam from a gynecologist in Layton, and would like to make an OBGYN appointment, our Utah OBGYNs are currently accepting new patients. OBGYNs (obstetrician-gynecologists) provide annual checkups for women as well as treatment for pelvic, vulvar, and vaginal pain, vaginal bleeding, breast care, family planning, pregnancy checkups, and even more. Tanner Clinic has both obstetricians and gynecologists, as well as individuals who are experienced in both fields. We provide complete routine physical exams with each annual appointment and make sure that your reproductive system is as healthy as can be. For women attempting to conceive who are at a higher risk due to a condition like gestational diabetes, we have maternal-fetal medicine doctors or MFM specialists. Their particular medicinal training is in the health of both mother and child in difficult pregnancies. Additionally, we offer cancer screenings for breast, ovarian, uterine, and cervical cancer. These are crucial screenings for any woman, since the symptoms can oftentimes present as something relatively innocuous. Building a relationship with an OBGYN and making regular visits could mean the difference between an early diagnosis and one that comes after an illness has progressed.
Some of our other services include:
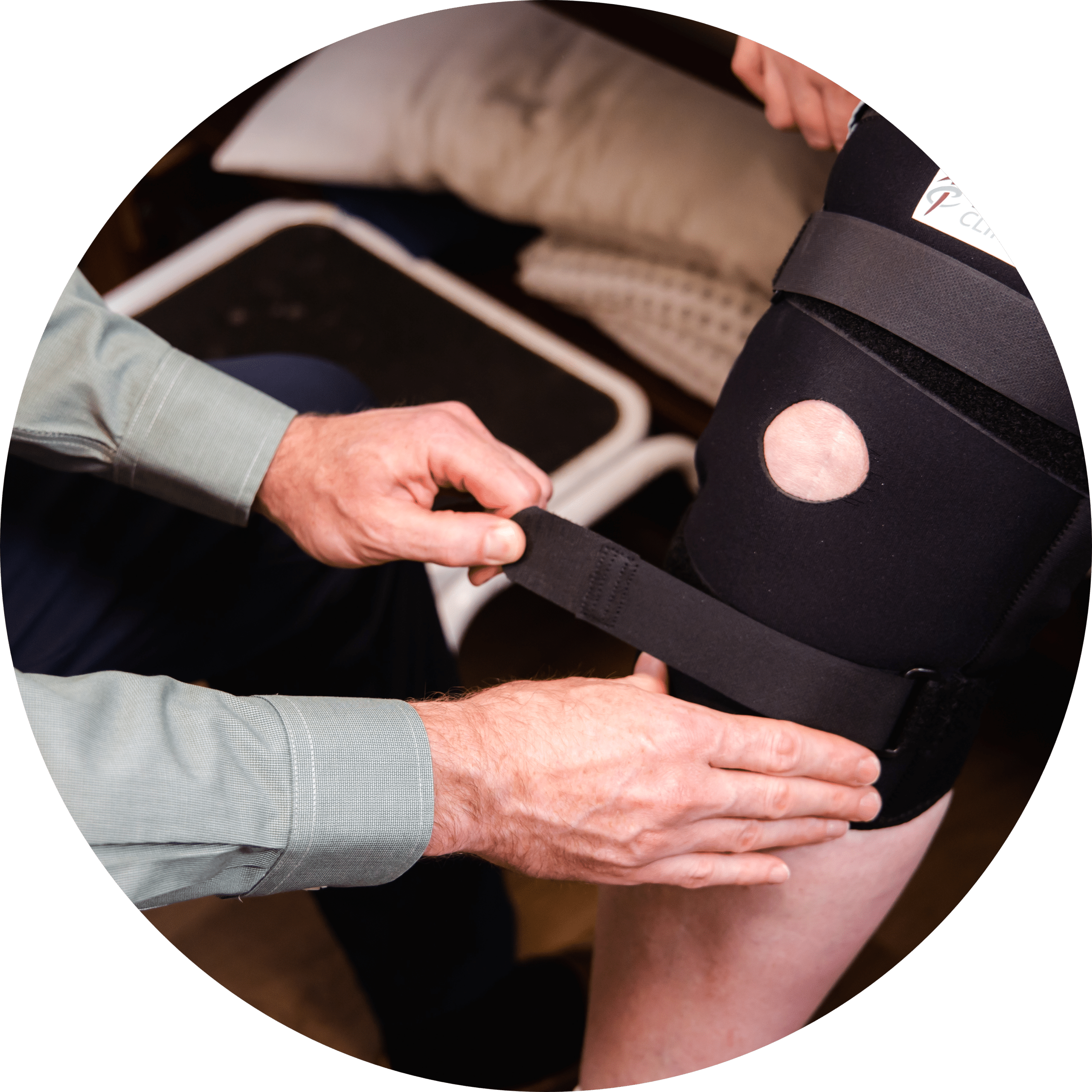
Orthopedics is the branch of medicine that treats and diagnoses injuries or disorders of the skeletal system and associated muscles, joints, and ligaments. They also treat chronic problems, such as long-term tendon, muscle, or joint pain. From surgeries to simple fixes, orthopedic surgeons and orthopedic doctors handle a wide range of musculoskeletal conditions. We have orthopedic providers at these locations:
Sports injuries are among the most common orthopedic injuries that we treat, so our sports medicine physicians work closely with our orthopedic providers to communicate and provide innovative treatment options. Specialized procedures are available at our three clinics that have orthopedic providers; we make sure that whatever procedure we choose will have the best outcome for you as a patient. Some of the common conditions we treat include:
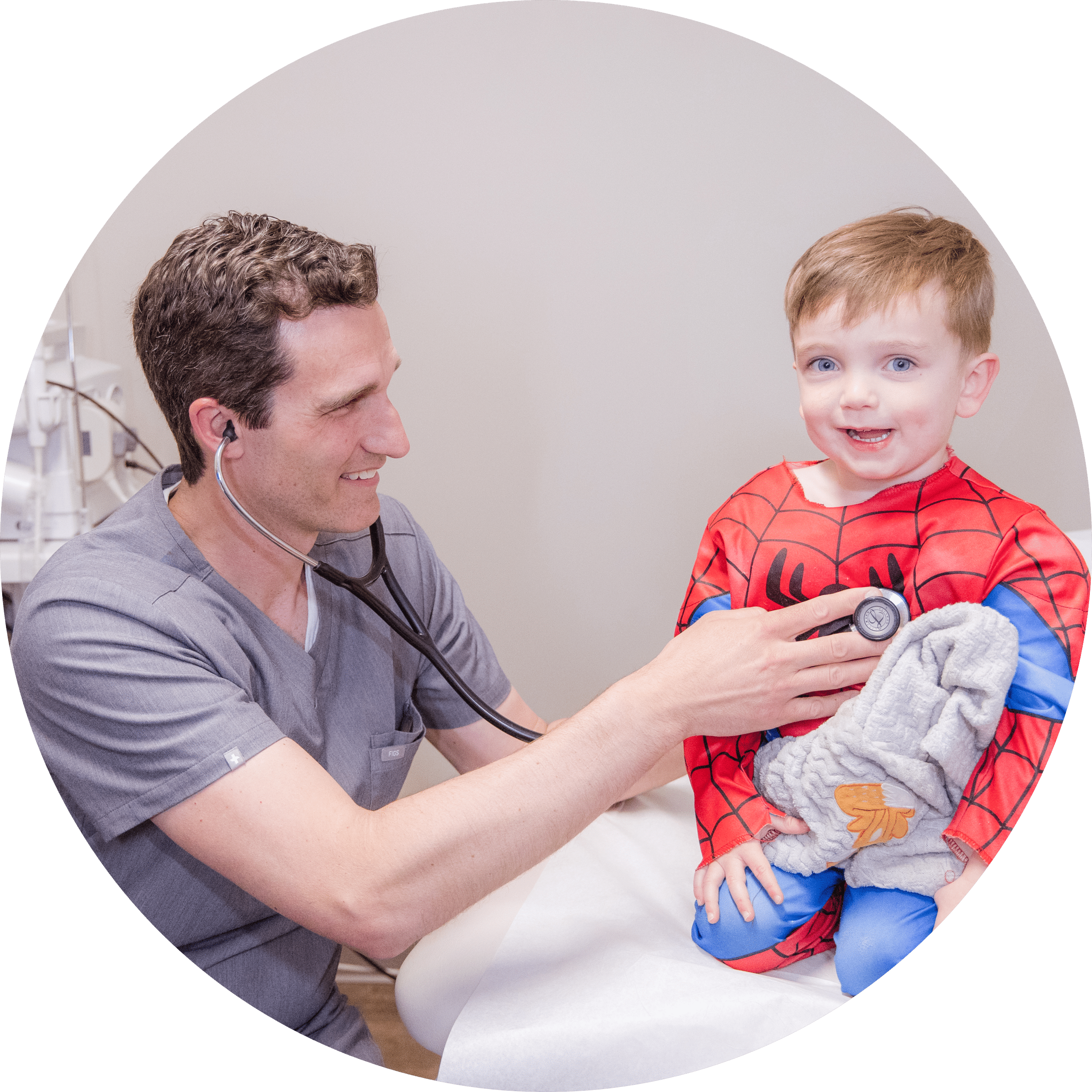
Specialists that work closely with our family medicine doctors, pediatricians specialize in treating medical and behavioral conditions for infants, children, and adolescents. We provide comprehensive, individualized healthcare to children at any point in their development, both on a routine basis – vaccinations, well-checks, and seasonal allergies – and in the event of a more serious circumstance such as a broken bone or a fever. Our goal is to find long-term solutions to keep your child healthy all year long.
Along with our other specialists, Dr. Candice Smith is a pediatric infectious disease specialist with Tanner Clinic. Infectious disease specialists address infections from bacteria, viruses, parasites, or fungus that seem persistent or severe for your child. Dr. Smith treats several conditions, including:
